Once again it has been an inordinate length of time since I last posted anything here – in fact, it’ll be getting on for two years in another month or so.
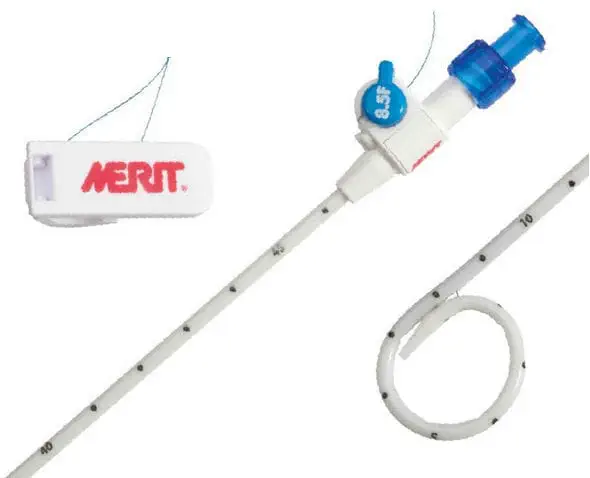
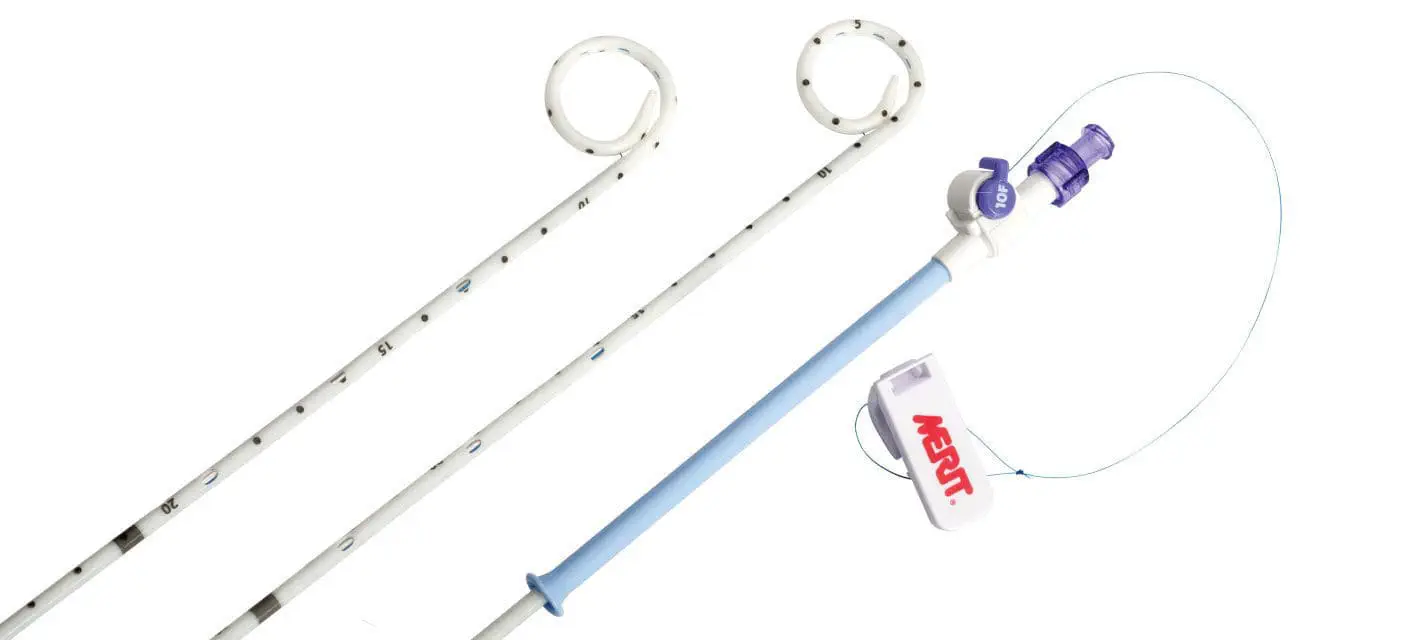
Those who follow my (very!) occasional ramblings will recall that the last time I added anything to this oft-neglected chronicle, I had just spent three months “enjoying” the experience of having about 15cm of plastic tubing (see below) stuck in my abdomen. This new bit of internal plumbing was then connected to a bag that I had to carry around with me in order to drain the poisonous contents of a severely infected gallbladder that was, at one point, threatening to send me off to the Pearly Gates/Pits of Hell (delete as applicable).

Obviously, that didn’t happen (phew!) but it was an unpleasant time nevertheless. At the beginning of October 2022, when the surgeons made the decision to remove the gallbladder drain, I was about five or six weeks out from having my gallbladder removed (surgery was scheduled for mid November 2022). According to the surgical team, my various scans and other tests suggested that I should be fine without the drain for that length of time so it was just a case of going home, recovering from having the extra pipework and then returning to hospital to get the troublesome little organ evicted once and for all.
Oh well. As it turned out, these were what are usually known as “famous last words”. I lasted about two and a half weeks before my temperature started climbing, the nasty abdominal pains started up and I once again found myself beginning to shake, shiver and lose touch with reality a bit. So it’s off we go to A&E in Stranraer and, while I waited to be triaged and checked out, Glenda popped back home to pack me a bag. We knew full well that I’d be off to the Costa del Dumfries and Galloway Royal Infirmary once again. As soon as the doctor saw me, he agreed and they confined me to a nice quiet room with various needles, medications and drips stuck in my arms, to await transfer.

I reached DGRI on a dark Friday evening and, after waiting around for a while to be checked in by the A&E staff, I was whisked off to the surgical ward once again. The next day, after some tests and a bit of prodding and poking, the surgeon came in to tell me that, this time, it was too risky NOT to operate so I’d be scheduled for emergency surgery on the Sunday. The only thing that would stop it happening would be if some major disaster befell and all the operating theatres were full of other people being put back together.
That particular scenario didn’t come to pass, so I duly found myself wheeled away to the big shiny room on the Sunday afternoon. Glenda, meanwhile, was stuck waiting for me and gnawing her fingernails down to the elbows, having been party to the surgeon and anaesthetist giving me the usual run-down of all the ways that it might go terribly wrong and getting me to sign the relevant “I know what I’m letting myself in for” paperwork.
After the first few minutes in theatre, admiring all the hi-tech machinery and the glowing lights and big screens and what have you, one of the nice masked people told me to take a whiff of this, injected something into my arms and my brain proceeded to wander off and play with the fairies for a few hours. By the time I recovered, I was en route back to my hospital room (still rather groggy and largely out of it), but with a few new holes scattered around my abdomen and one gallbladder missing, presumed chucked in a medical waste bucket somewhere. Yay!
Of course, in typical fashion, I had chosen the worst possible time for all this. The following day (Monday) was Glenda’s dad’s funeral and we were supposed to be there and I was supposed to be doing one of the readings. Obviously this couldn’t happen, but knowing that I had come through the surgery and – while not exactly feeling tip-top – was at least alive and likely to recover, Glenda travelled down to Kendal with some of the other members of the family and attended the service. The wonderful nurses on the surgical ward even made sure that I was given some privacy in my room so that I could watch a live-stream of the proceedings on my iPad that afternoon.

Now, normally following gallbladder removal, you’ll be sent home very quickly – sometimes the same day, otherwise the day after the operation. However, in my case, it had all been a bit, well, icky and horrible in there with infections and other assorted nasty things, so I’d had to be mauled about more than usual and ended up with a slightly non-standard removal. The practical upshot was that various of my internal parts shut down in protest (something called Post-operative Paralytic Ileus for the medically inclined) and I proceeded to be rather unwell for the rest of the week. This included the delights of a naso-gastric tube for a few days and not really knowing when (or even if) the onboard systems of the USS Adrian were likely to reboot themselves and start working again. And, having been away at a family gathering with a couple of hundred people, poor Glenda was unable to take the risk of coming in to see me in case she brought cold, flu, COVID or other assorted bugs with her.
That was, if you’ll excuse the expression, a really, really shite week for us both.
However, by the Friday, things were looking up, the NG tube was removed and on the Saturday I was deemed fit enough for discharge. Woohoo! One 80-odd mile taxi journey later and I was back home, where Glenda had done stalwart work cleaning the house, tidying up and preparing for the doddering old invalid to take to his bed and continue his recovery. And so it came to pass. The first few weeks weren’t that much fun and largely consisted of resting and consuming regular doses of morphine to stop me going “Ouch! Lawks! Yarroooo!” whenever I tried to move too much. But time passed, I got better and started going for short – very, very slow! – walks. I then took longer walks and, after maybe six months, things were looking up.
Which was when it all seemed to go a bit runny again and I found myself not actually ill, but lacking in energy and failing to recover my previous strength and stamina. And that is still how I find myself today. While I’m theoretically recovered from the surgery and all the gallbladder-related nastiness, I’m still not quite my old self. This is bloody annoying to say the least and I’ll admit that it has taken a bit of a toll on my mental health over the last year or so. I’m still trying to find my way through it really.
But – and it’s an important but – I’m still here. I might even have the time to write a bit more. (Yeah, yeah, we’ve all heard that before…)